Workers recovering from COVID-19 or influenza may experience a range of complications that might prevent their return to work. In this article, we offer some tips to support your employees’ safe return to work after recovering from these illnesses.
COVID-19, Long COVID and Influenza
With the cool winter months well and truly setting in, the chance of catching influenza (the flu) or COVID-19 is higher. Australian state health authorities are reporting increased levels of COVID-19 in the community and hospitalisations this season so now is the time to refresh our knowledge of these diseases and how we can support our workers.
COVID-19 and the flu are caused by different viruses and can have varying levels of severity and long-term impacts. Although most people recover from COVID-19 and the flu within a week or two, a small percentage of people might have ongoing symptoms after weeks or months.
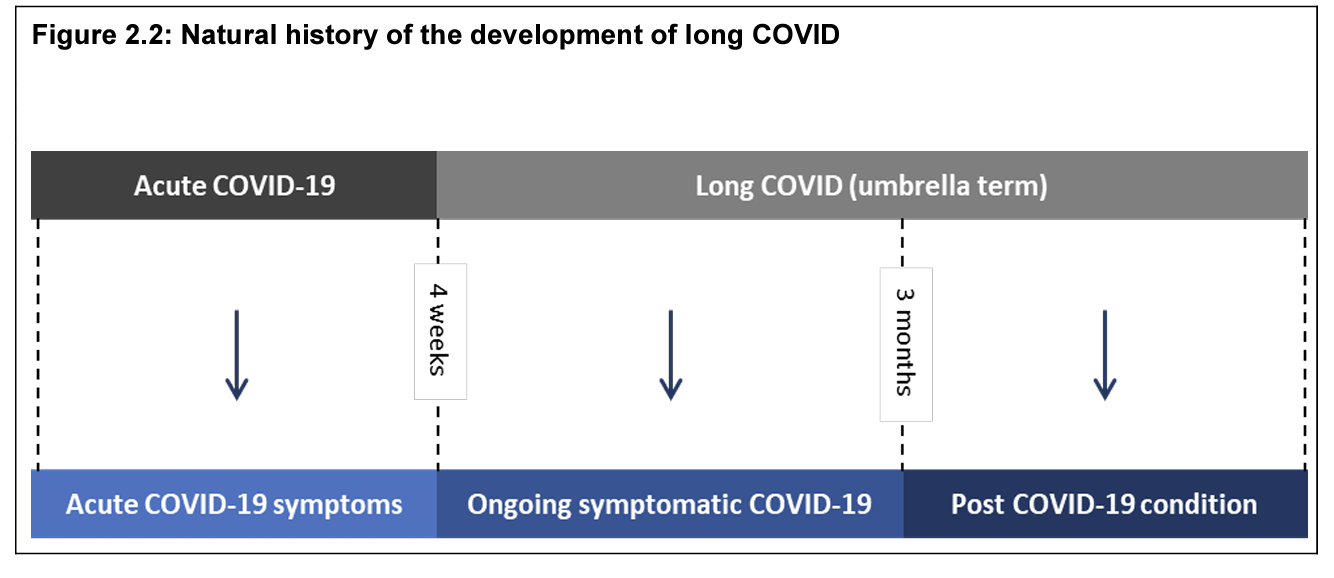
Long COVID refers to the prolonged symptoms experienced after recovering from COVID-19. Around 5–10% of COVID-19 cases in Australia reported symptoms persisting for more than 3 months. It is also possible to suffer long-term effects from the flu, although the risk is not as high compared to COVID-19.
Most workers with ongoing symptoms will need modifications to be made in the workplace. Some workers, especially those in heavy manual roles, may need to return to work gradually, building up their work capacity over a longer period.
Long-term effects from COVID and influenza can include:
- Fatigue, brain fog
- Cough, feeling short of breath or chest pain
- Joint or muscle pain
- Change in sense of taste or smell
- Anxiety and/or low mood
- Trouble sleeping
Persisting symptoms can impact daily activities and workforce participation, “including delays in return to work, and ongoing residual difficulties that impact the ability to perform the same duties or limit working hours.” (Australian Institute of Health and Welfare)
How to support your employees
Some barriers to patient motivation in their recovery can be grouped as personal and workplace barriers.
1 – Check in and stay in touch while the worker is absent from work. Let them know you are there to help and support.
Consider a return-to-work plan for workers who have had severe COVID-19 or influenza. Some workers may experience on-going symptoms and may take longer to be able to work at the same level as before. Arrange a meeting with the returning worker to establish a return-to-work plan.
- Take time to check in with returning workers; ask how they are and if there is anything they are struggling with.
- Consider possible modifications to their job and work schedule for the first weeks of their return.
- Agree on a return-to-work plan that you are both comfortable with.
- Monitor and review how things are progressing.
2 – Provide support during the early days after return to work
Give them permission to take things slowly to start with, as this will prevent them from feeling overwhelmed and reduce the risk of further absence.
Remind them of the work schedule and job modifications you have agreed on and check these are in place and working well.
Arrange regular check-ins to talk through how they are managing their health and work.
3 – Provide ongoing support and review regularly
Review workloads and agree to gradually increase the duties over the coming weeks or months. For a few people, COVID-19 infection, influenza and long COVID symptoms may mean that the worker is unable to meet the requirements of the job — if so, you may need to consider a change of duties.
It is also important to keep an eye on the workload of other workers. The absence or reduced work ability of a substantial number of workers may cause a strain on the remaining workers. Keep any additional workload as low as possible and ensure that it does not last too long. Line managers have an important role in monitoring their workers and ensuring that individuals are not overworked.
4 – Develop job modifications if required
Modifications should be tailored to the individual and will depend on what their specific symptoms and limitations are and how these affect their ability to perform the requirements of their role.
For workers with fatigue symptoms, remote working and ‘pacing’ (i.e., working with rest breaks as determined by symptoms) can be helpful. Some workers may be able to continue their full hours; for others, a planned reduction of working hours could be more effective.
Individualised recovery and rehabilitation plans may be required, this can include:
- Adjustments to start and finish times and breaks
- Adjustments to work hours, e.g., shorter days, days off between workdays
- Adjustments to shift work, e.g., consider suspending late or early shifts and/or night duty, so the individual works when at their best
- Modifications to work patterns, e.g., pacing, regular and/or additional breaks
- Modifications to workload
- Temporary changes to duties or tasks
Workers may also be at risk of de-conditioning, particularly those who may be having extended periods of leave and those who have been in isolation. These workers may have an increased risk of injury upon their return to work.
Your Workplace Health Provider can assist workers experiencing symptoms of muscle and joint pain and can develop tailored strength and conditioning programs to ensure de-conditioned workers are fit for the task.
Further resources:
COVID-19 business and organisation kit. Department of Health and Aged Care.
Understanding post-COVID-19 symptoms and long COVID. Health Direct.
Long COVID in Australia – a review of the literature. Australian Institute of Health and Welfare.
Sign up to our monthly enewsletter
"*" indicates required fields